
Want to improve your Brain Function even further?

In my last column, we discussed “Cognitive decline as you age and its preventive measures.” Now, let’s take this one step further. I want to introduce you to two new concepts – “How can we repair and restore brain function after an injury?” and “How to improve an already healthy brain even further?” Your brain, as healthy as it may be, can be improved or at least preserved the way it is for a considerable period of time. And to an extent even after developing a major disease like stroke, multiple sclerosis or traumatic brain injuries (TBD).
Conventional wisdom was that once a person attains maturity, the brain cannot improve much functionally. So, if a person suffered an injury or developed a psychological problem that did not improve, the impression was that the brain is “hard wired” (a metaphor suggesting that the brain has permanent neurological circuits that couldn’t be altered as in a computer, designated to perform a specific but unchangeable function).
Scientists at the frontiers of brain research have shown that the “brain can change its very structure with each different activity perfecting its circuits so it becomes better suited to the task at hand.” And if certain parts failed, other parts could take over. So, if brain cells die, the brain has the potential to regenerate and replace those cells. The process may not happen quickly or in large amounts and not necessarily in all areas. But something is better than nothing, right?
This phenomenon of ‘neural regeneration’ tends to occur primarily in two specific areas of the brain – the hippocampus, the region involved in learning and memory and, within areas of cerebral cortex where lesions responsible for strokes tend to occur. Re-establishing connectivity between new cells and the existing array of neurons – reorganization of spared areas and pathways in these neurogenic regions leading to plastic remodeling – is called neuroplasticity.
This concept of neuroplasticity has found its practical application in the rehabilitation of stroke victims. Stroke remains one of the most devastating of all neurological diseases causing a severe damage to the very structure of the brain and its function. Although emergency treatment can minimize this damage, once the stroke is established, it results in considerable disability including paralysis of the limbs. About 80 percent of these survivors have significant motor impairments, especially of the upper limb that gravely affect their ability to perform activities needed for daily living. And some have hemiplegia or hemiparesis affecting one-half of the body. Improving this paralysis is of utmost importance to maintain basic daily activities.
Conventional physical therapy can improve the muscle weakness but only up to a point. However, a new neuroplasticity-based treatment invented by Edward Taub, Ph.D, a behavioral neuroscientist, promises to change all that. Taub and his team of research scientists working at University of Alabama have developed over the past 25 years a special type of rehabilitation therapy called Constraint-Induced Movement Therapy (CIMT) “designed to help ‘rewire’ the brain and thus regain some level of limb function in those who have had an insult or illness such as traumatic brain injury (TBI), stroke, brain tumor, or even multiple sclerosis.” In other words, these patients can relearn to improve the function of the affected parts of their bodies (like the paralyzed limb) rather than depending on the less-affected or normal parts.
The basic premise of CIMT is that if the patients were forced to use the paralyzed limb by purposeful immobilization of the better or normal limb that could lead to improvement of the function in the affected limb. This means, with enforced restriction or even immobilization of the normal limb, the patients soon learn to live with the constraint and start using the diseased limb more and more. Taub’s contention was the affected limb may develop ‘disuse atrophy’ if not put to ‘forced use’ and the way to prevent it is by ‘forcibly constraining’ the good limb.
Brain imaging studies have confirmed CIMT’s beneficial effect indicating that there is indeed “rewiring” of the brain taking place and this translates into clinically significant improvement in the strength and movement of the affected limb. As Edward Taub, Ph.D., says, “Each year, hundreds of thousands of patients experience strokes in the U.S. alone. New behavioral interventions, like CIMT, give these patients hope that they can overcome their challenges.”
Reference: The BRAIN that changes ITSELF by Norman Doidge, M.D.
M.P. Ravindra Nathan, M.D., is a cardiologist and Emeritus Editor of AAPI Journal. His book “Stories from My Heart” was recently released. (www.amazon.com or www.bn.com).
EYE CARE
FIXING LASIK COMPLICATIONS: Back to 20/20 (PART I)

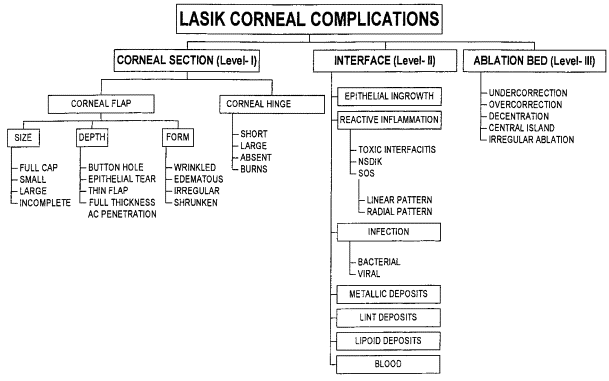
Gulani AC. Ophthalmology: Journal of the American Academy of Ophthalmology, August, 1999
Having honed Lasik surgery over nearly three decades to a “non-cutting” technique, most complications are not relevant anymore in the present times. More importantly, I believe that most Lasik complications can be corrected back to 20/20.
Having worked with excimer lasers (laser used for Lasik surgery) in the early 1990s, much before many surgeons in the world (U.S. FDA gained approval in 1994), I had seen the impact of Lasik on the future of vision for millions of patients without glasses. I also realized that the talent required for consistently safe and predictable results lied with a good understanding of the cornea and the laser itself to then modify algorithms to each patient individually.
Two decades ago, I had published in the Journal of the American Academy of Ophthalmology my take on how Lasik complications would become a reality given that so many surgeons were jumping on the bandwagon without adequate training or corneal surgical experience. Add to that, advertising hype and financial deals, and it was a perfect storm in the making.
In previous two columns, we reviewed Lasik complication incidence and presence worldwide in lieu of the New York Times article. Given the tremendous interest from the readers, I have decided to review my approach to correcting Lasik complications in the next two columns.
Even though my classification system was published two decades ago, it holds true till date that my predicted proposal to align complications with treatment plans would be in use by surgeons globally.
So, in following the same outlay, lets in this column address the level I complications and patient complaints associated with it
All of level I complications as you can see are related to making the Lasik flap (cut in the cornea). These variants of complications are named as per the level of damage and actually this incidence of Level I complications dramatically decreased with introduction of Femtosecond lasers (Bladeless), which have replaced many microkeratome (blade used for cut) Lasik outfits.
Nevertheless, lasers can also have their shortcomings and inflammation levels can be higher as well as suction breaks due to anatomical difficulties.
Most Level I complications can result in patient symptoms of vision distortion, fluctuating vision, dry eyes, pain, night vision issues, double vision and haloes/starbursts.
Treatment approaches for Level I complications is where I teach Lasik surgeons to have a solid foundation of corneal anatomy and surgical experience since most of these complications are related to a finally unstable and irregular cornea.
In cases of limited corneal damage, one can allow adequate healing time to then be followed up by realigning the Lasik flap, for example, in cases of flap wrinkles and macro striae with or without glue/sealants. Excimer laser can be used to also smooth the anterior surface of a superficially damaged flap.
In cases of moderate flap damage, one can suture the flap to align and fixate as well as re-lift to re-approximate using special instruments (Gulani Lasik complication management instrument set - Bausch & Lomb) to secure the anatomy.
When there is severe corneal damage from flap accidents, one can remove the flap and replace with donor cornea (without suture or do an automated lamellar keratoplasty) or replace the flap tissue with a hand dissected lamellar graft (partial graft). In even more severe case, one can do a deep anterior lamellar keratoplasty (DALK) surgery.
Dry eyes can be scientifically approached with unique combination treatments successfully while adjunctive and elegant surgeries like INTACS can be used for herniating corneas (ectasia) and amniotic tissue (human placenta) can be used to accelerate healing and stabilize the cornea.
Most important, after rehabilitating the cornea, the same Lasik laser can be used in Corneoplastique mode to then shape the newly stabilized cornea to bring the patient back to vision and, in many cases, 20/20 without glasses.
Of course, non-surgical modalities like specialty contact lenses, including scleral contact lenses, can be used for Level I complications. But surgical intervention may be needed in most cases and by following the above algorithm, it is possible to reverse majority of the patients back to 20/20.
In the next column, I shall review Level II complications and management.
Arun C. Gulani, M.D., M.S., is director and chief surgeon of Gulani Vision Institute in Jacksonville. He can be reached at [email protected] or visit www.gulanivision.com